from the Perelman School of Medicine at the University of Pennsylvania, the current method for assessing damage to liver drug-related does not provide an accurate picture of the toxicity of certain drugs, or lack thereof.
New approach identifies the most toxic drugs for the liver
The classification of a drug’s potential harm to the liver, called “hepatotoxicity,” has historically been determined by counting individual reported cases of acute liver injury (ALI). Instead, the researchers used real-world health data to measure ALI rates within a population and found that the liver-threatening levels of some drugs are misclassified. Their article was published on JAMA Internal Medicine .
“From a clinical perspective, knowing the rate of severe ALI after starting treatment based on real-world data will help determine which patients should be monitored more closely with liver-related laboratory tests during treatment,” he said. said senior author Vincent Lo Re, MD, MSCE, associate professor of Medicine and Epidemiology.
“Incidence rates of severe ALI can be a valuable tool in determining a drug’s liver toxicity and when patients should be monitored, as incidence rates provide a truer and truer view of this toxicity. Case reports did not accurately reflect observed rates of ALI because they did not consider the number of people exposed to a drug, and cases of drug-induced liver injury are often underreported.”
As part of the study, 17 different drugs had rates that exceeded five serious ALI events per 10,000 “person-years,” a measure that reflects both how many people are in a group and how long the study observes them (12 years -person could mean one person with data covering 12 years or two people covering six years).
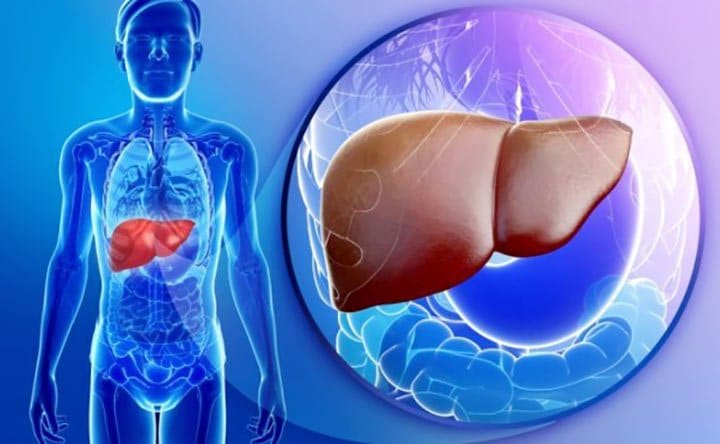
The team determined that 11 of these drugs fell into lower categories of hepatotoxicity based on case counts that likely did not reflect their true risk, as their incidence rates revealed higher levels of toxicity.
One of the drugs that fell into this group was metronidazole, an antimicrobial that can be used to treat infections in the reproductive or gastrointestinal systems, as well as some dermatological conditions.
Incidence rates, the number of new cases of a disease over a period of time divided by the number of people at risk of the disease, are a key measure for examining the health of a population because they provide a more complete picture than simply count.
For example, a drug with 60 reports of liver injury would be considered the most hepatotoxic by the traditional method, using the raw number of reported liver injury cases.
If that drug had seen 60 serious ALI events and was used by five million people, the incidence rate would be very low and would likely indicate that the drug is not dangerous to the liver. However, if 60 severe ALI events were observed in a population of 1,000 patients, this would reflect a higher, potentially more important injury rate.
To determine incidence rates, Lo Re and his team, including lead author Jessie Torgersen, MD, MHS, MSCE, assistant professor of medicine, examined electronic health record data from nearly 8 million people provided by the United States Veterans Health Administration that were compiled from 2000 to 2021.
Each person did not have pre-existing liver or biliary disease (a condition that affects the bile ducts or gallbladder) when they started taking any of the 194 drugs studied.
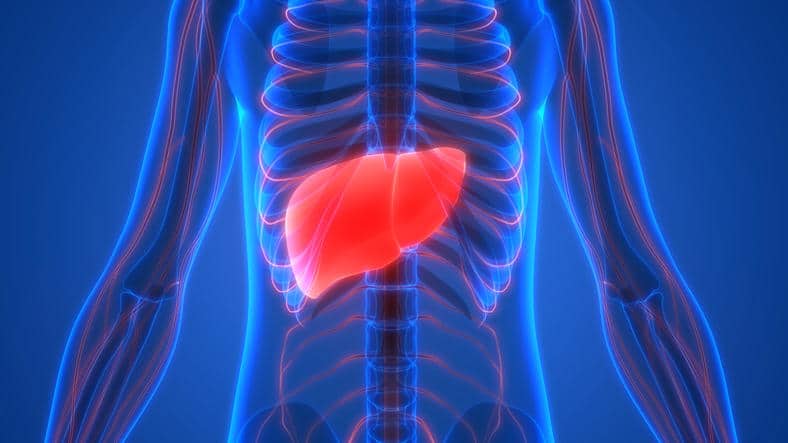
Each of these drugs was investigated because they were suspected of causing liver damage, as each had more than four published reports of liver toxicity associated with their use.
On the other side of the hepatotoxicity coin, the researchers found eight drugs that were classified as the most hepatotoxic based on the number of published case reports, but which should actually belong to the least liver-toxic group, with rates of incidence lower than a severe case. ALI event per 10,000 person-years. For example, rates of severe ALI for statins, often used for high cholesterol, were in the group that had fewer than one event per 10,000 person-years.
“The systematic approach we developed allows effective measurement of liver toxicity rates after initiation of drug therapy,” said Lo Re. “It was not surprising that clinical case counts did not accurately reflect the observed rates of severe acute liver damage, given the intrinsic limitations of clinical cases”.
With these findings, the researchers hope that mechanisms can soon be established within electronic health records to alert physicians to closely monitor the liver-related laboratory tests of patients starting treatment with an observed high rate of severe ALI.
“Importantly, our approach offers a method to enable regulatory agencies and the pharmaceutical industry to systematically investigate reports of drug-induced ALI in large populations,” Lo Re said.
A new patch could help treat and prevent liver disease
As described in research published in the Biotechnology Journal, researchers have developed a new patch that can aid the regeneration of liver tissue.
The patch is a combination of decellularized liver matrix, a hepatic growth factor, and an anticoagulant. In laboratory tests with liver cells, the patch helped liver cells resume function after exposure to a toxin.
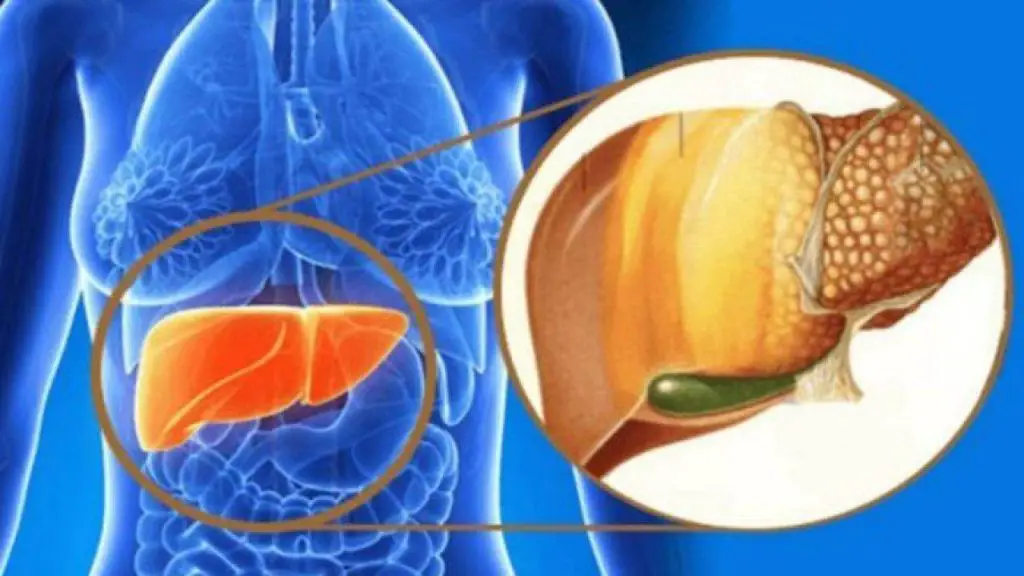
In rats, patches attached to the liver and intestines promoted recovery from liver fibrosis, with notable decreases in scarring and inflammation.
“The decellularized liver matrix-based liver patch demonstrated the ability to restore liver function and inhibit inflammation in fibrotic livers,” said corresponding author Yung-Te Hou, Ph.D., of the National University of Taiwan. “This approach shows great potential for treating various liver-related diseases, ranging from mild conditions such as fatty liver to severe conditions such as liver cirrhosis.”
New stem cell research could have implications for liver transplantation
Liver disease, due to viral infections, alcohol abuse, obesity or cancer, accounts for 1 in 25 deaths worldwide. A liver transplant can save the lives of people with end-stage liver disease. However, the procedure has limitations related to donor shortages, a technically demanding and invasive surgical procedure, and the need for lifelong immunosuppressive drugs in transplant recipients.
An alternative to whole organ transplantation is the less invasive injection of dissociated human liver cells, but donor shortages are still a problem. Using interspecies blastocyst complementation to obtain transplantable human liver cells or entire organs in sufficient quantities in a different animal species was one way to overcome these barriers.

An important question is whether liver cells cultured in a different species would be fully functional. To find out, Wei Li and colleagues at the Chinese Academy of Sciences in Beijing injected mouse embryonic stem cells into early rat embryos. The rat-mouse chimeras born from these engineered embryos contained mouse cells in most parts of the body, including the liver.
The percentage of live mouse liver cells enriched was up to 20.6% from chimeric livers. Encouragingly, mouse liver cells cultured in rat-mouse chimeras exhibited normal appearance and mature function in a laboratory test panel. Furthermore, mouse liver cells from rat-mouse chimeras could be transplanted into mice with liver damage and had a therapeutic effect similar to that of normal mouse liver cells in alleviating chronic liver fibrosis.
These data, recently published in the journal Stem Cell Reports , provide proof of principle that functional liver cells can be grown in a different species and could provide a solution to the transplant shortage. Future work is needed to develop efficient techniques to grow human liver cells in large animals such as pigs and to investigate whether these human liver cells are fully functional.
#Liver #precisely #identify #toxic #drugs














