A team of scientists from the University of Manchester have shown that testing for two gene families linked to a risk of ovarian cancer epithelial between 5% and 20% have a much higher than expected detection rate. Routine testing for mutations in homologous recombination (HR) and mismatch repair (MMR) genes in women with the disease who also have a family history of ovarian, breast and other cancers would save lives, they say.
The results of the Research have been published in the scientific journal Genetics in Medicine.
Routine testing for ovarian cancer: etc. why they are important
The new research is the largest to date on cancer causing genetic mutations in ovarian cancer. The research team tested 277 women with ovarian cancer whose close relatives had been diagnosed with the disease in their lifetime. Of those who tested negative for BRCA1 and 2 gene mutations, 22% were positive for HR and MMR, twice the equivalent detection rate in breast cancer.
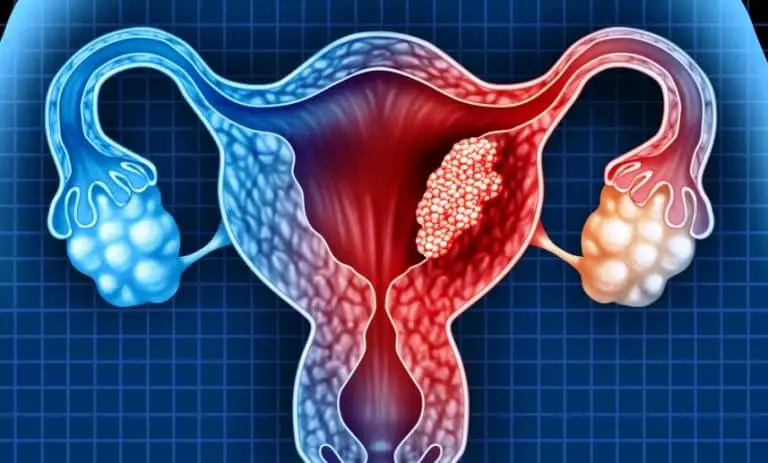
Currently, doctors routinely test the cancer-causing genes BRCA1 and BRCA2 which are associated with a lifetime risk of 20% to 60% and 10% to 25% respectively. However, although they do test for other genes, it’s not a routine. HR genes work in conjunction with BRCA genes, and MMR genes are associated with Lynch syndrome, a condition passed on from parents to children that increases the risk of several types of cancer. One of the HR genes, known as BRIP1, was the only gene responsible for most cancers after BRCA1 and BRCA2.
Identifying mutations in people with advanced ovarian cancer could allow doctors to prescribe them personalized gene therapies that specifically target the cancer. And detecting faulty genes in close relatives who are doing well, such as daughters, grandchildren, aunts or cousins, could give them the chance to reduce their risk with preventative surgery.
Dr Nicola Flaum, lead author of the University of Manchester study, said: “This project is the most detailed genetic study to date on familial ovarian cancer. And we show that two families of genes with a lifetime risk of epithelial ovarian cancer of between 5% and 20% are even more present in these families than we thought. “
“That’s why we think that as a matter of routine, women who are BRCA1 and BRCA2 negative with a family history of ovarian, breast and other cancers should be tested for these other genetic mutations. Wider genetic tests on women with familial ovarian cancer are essential both to optimize their treatment and to enable disease prevention in family members ”.
The scientist added: “Ovarian cancer has a poor survival rate as it is usually diagnosed late. That is why it is important to test even asymptomatic family members so that risk management strategies can be offered. We urge patients to tell doctors their family history so that they and their relatives can be tested. “
Dr. Ilaria Betella of Surgical Gynecology of the European Institute of Oncology in Milan, said: “It is estimated that up to 15-20% of ovarian cancers are linked to the presence of mutations in the BRCA1 and BRCA2 genes. But if we also consider other hereditary syndromes, the share of hereditary ovarian tumors on the total could reach 25-30% ”.
“Studies to date have shown that lifetime risk of developing ovarian cancer and the age of onset vary depending on the mutated gene. In the case of BRCA1, the risk is between 40 and 60%, while for BRCA2 it drops to 20-40%, with a slightly older age of onset than BRCA1. Genes involved in the development of Lynch syndrome can also predispose to ovarian cancer, for example in the presence of germline mutations of the MSH2 gene the risk ranges from 8 to 38% over the course of life, with an average age at diagnosis of 43 years. , while in the case of alterations in the MSH6 gene the risk is 1-13%, with an average age of onset of 46 years “.
“Ovarian cancer is a pathology that actually encompasses different neoplasms and over time significant progress has been made both in diagnosis and in therapy. «Today precision medicine is predominantly part of the diagnosis of this tumor – explains Betella -. In the last 20 years enormous progress has been made which has led to the possibility of carrying out genetic and molecular tests in practically all patients ”.
“From a clinical point of view, this has resulted in the widespread search for BRCA mutations in all patients with ovarian cancer in the last 6-7 years. In 2019, the Manchester Consensus led to the indication to screen for Lynch syndrome in some particular subgroups of ovarian cancer (in particular endometrioid and clear cell) ”.
“In the case of women with BRCA mutations who have now developed ovarian cancer (as well as for another group of patients, ie those who have a sporadic tumor but whose tumor develops somatic mutations in the BRCA genes) today we can use PARP inhibitors, drugs that have significantly improved prognosis, extending survival “.
“This has certainly had a positive impact on the quality of life, but we must not forget that these are women who have to deal with a diagnosis that changes their life forever, not only for the type of cancer, but also for the type of surgery that requires “.
“After this type of more invasive surgery some physiological aspects change, for example many patients report that their intestines work differently or complain of other problems, with which they survive and with which we must learn to live with”, added Betella.

“The good news is that PARP inhibitors are very well tolerated drugs, although there is a need for the patient to have blood tests periodically because they sometimes cause anemia, a reduction in white blood cells or platelets. Furthermore, having to perform periodic examinations, the patient is led to think about her pathology more frequently ”.
“Despite this, we have seen that patients are in favor of taking PARP inhibitors: knowing their benefits, they are able to better tolerate any side effects. Sometimes it is necessary to adapt the dosage of these drugs to the individual patient, in order to allow her to manage nausea, weakness and haematological effects, which are the most frequent side effects and usually reported in the first periods of taking the therapy “.
“Today we know that, in a healthy woman with BRCA mutation who undergoes prophylactic annexationectomy, it is absolutely possible to have hormone replacement therapy safely. More recent studies do not show an increased risk of developing breast cancer. We must bear in mind that most BRCA-related breast cancers do not have hormone receptors and therefore are not stimulated by the presence of hormones ”.
“However, different strategies can be put in place to improve the quality of life. For example, it is possible to resort to drugs that have positive effects on sleep or dietary measures and physical activity that help reduce hot flashes rather than local vaginal therapies to counteract dryness and improve sexual activity “.
“From the studies that have been conducted so far it has emerged that the patients who, before the prophylactic surgery, were explained in great detail the side effects of the surgery, are satisfied with the choice they have made (reduce the risk of neoplasia with surgery ) and considered the side effects more tolerable than in less informed patients “.
Studies are underway evaluating a two-stage prophylactic surgical approach on healthy high-risk women. In practice, it is a matter of first performing the salpingectomy (removal of the tubes) and then, after a few years, the prophylactic ovariectomy. Although the oncological safety of this approach is still to be confirmed, recent studies report its positive effects on the quality of life front ”.
“Studies are underway evaluating a two-stage prophylactic surgical approach on healthy, high-risk women. In practice, it is a matter of first performing the salpingectomy (removal of the tubes) and then, after a few years, the prophylactic ovariectomy. Although the oncological safety of this approach is still to be confirmed, recent studies report its positive effects on the quality of life front ”.
Salpingectomy is a minimally invasive surgery, performed in laparoscopy in which only the tubes are removed, which means that the patient will not be able to spontaneously get pregnant, but thanks to medically assisted procreation (MAP) techniques, she could still have a child , still having the ovaries and the uterus ”.
“This type of surgery may therefore be easier for women at high risk of developing ovarian cancer to accept and may be performed earlier than oophorectomy. However, this two-stage approach has not yet entered clinical practice and will only be able to do so when we have a defined picture of the cancer risk, only when we are sure that by proposing it to women we will not expose them to a higher residual risk of cancer than the companions who are undergo traditional prophylactic salpingo-oophorectomy ”, concluded Betella.
#Ovarian #cancer #routine #tests #genetic #mutations #important












