According to the commonly accepted model, the Alzheimer’s disease it is characterized by an inescapable sequence, from the accumulation of toxic proteins in the brain to dementia resulting from neurodegeneration. (1)
Although this deterministic sequence is sometimes true, it does not appear to be the case for all patients. Furthermore, the disappointing results of recently commercialized medicines have highlighted the need to reconsider this disease, which affects nearly 10 million people in Europe.
A European consortium of doctors and scientists, led byUniversity of Geneva (UNIGE) and the University Hospitals of Geneva (HUG), in Swiss, which also includes INSERM in France, analyzed the data presented in almost 200 studies previously published.
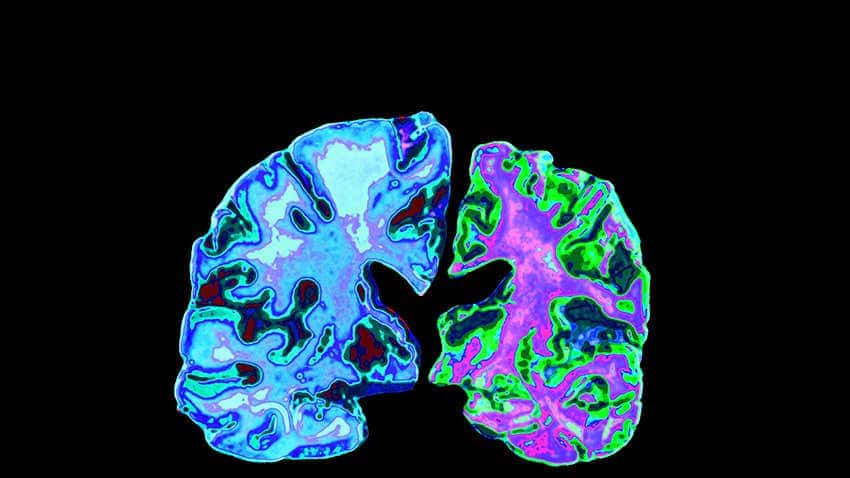
Far from being a monolithic disease in which the same causes produce the same effects, this analysis proposes a categorization of patients into three groups, each with its own dynamics. Furthermore, the research team calls for greater efforts to screen people at risk, in order to implement preventive measures as soon as possible.
This work, published in the scientific journal Nature Reviews Neuroscience, proposes a profound paradigm shift in the way Alzheimer’s disease is understood.
Alzheimer’s disease: that’s why it needs to be reevaluated
Alzheimer’s disease is usually described as a four-step sequence: an amyloid deposit appears in the cerebral cortex, so the hyperphosphorylated tau protein increases and aggregates in neurons. As a result, these dynamics cause neurodegeneration and ultimately cognitive decline, with memory loss being the first symptom.
The first drug targeting the deposition of amyloid plaques in the brain, approved a few months ago by European and American regulatory authorities, turned out to be relatively disappointing.: “Yet if we consider Alzheimer’s disease as a sequential cascade of biological events, it should have been much more effective“, explains Giovanni Frisoni, Professor of the Department of Rehabilitation and Geriatrics of the UNIGE Faculty of Medicine and Director of HUG Memory Center , who directed this work.
“Stop production of beta-amyloid with a drug it should logically stop the neuronal loss and thus the memory loss, which has not been observed massively. Furthermore, we found that some people with amyloid do not develop cognitive symptoms “, continued Frisoni.
To better understand why the deterministic model of disease is found in some cases but not others, the scientists conducted a systematic review of the literature., some articles tend to confirm this model, while others refute it.
“Our interpretative framework has shown that Alzheimer’s disease is more complex than it appears“, continues Daniele Altomare, researcher of the group of Giovanni Frisoni, who participated in this work. “Three groups of patients can be distinguished on the basis of their risk factors, the characteristics of their disease and their clinical fate “.
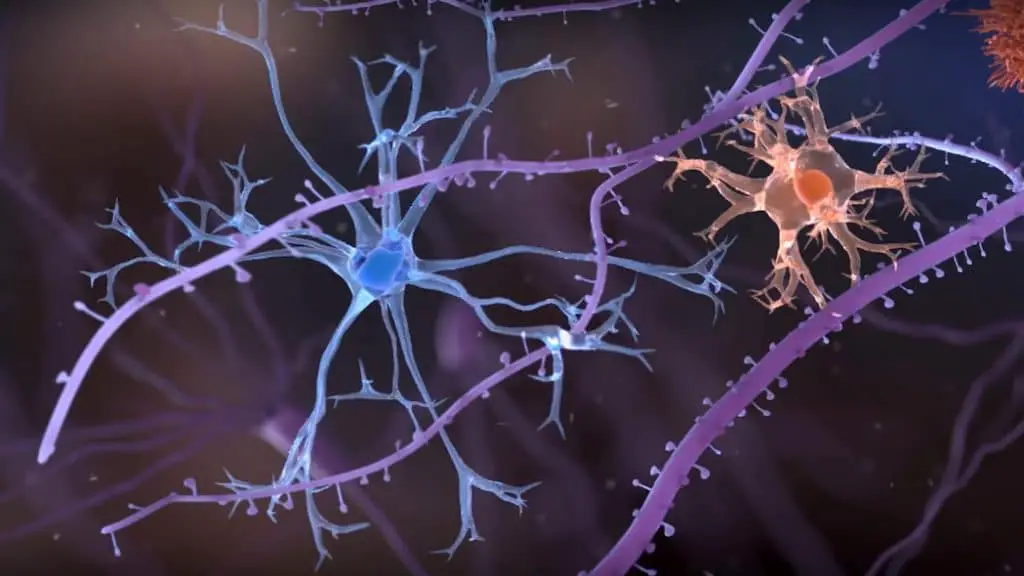
Therefore, the cascade forecast is confirmed only in one of these three groups, in which patients carry an inherited genetic mutation known as “autosomal dominant“. Fortunately, this mutation is rare, as it leads to the systematic development of early cognitive impairment (between 30 and 50 years of age).
In the sporadic form, the development of symptoms of cognitive impairment differs depending on the presence or absence of a genetic variation, the e4 allele of the APOE gene, which turns out to be an important risk factor: two thirds of carriers will develop the symptoms of Alzheimer’s disease sooner or later.
THEThe third group consists of people with no associated genetic mutation for which the presence of neurotoxic proteins seems to be an important but not unique risk factor: “Half of our patients belong to this third group“, Underlines Giovanni Frisoni. “Our probabilistic model therefore suggests that all genetic and environmental risk factors should be considered. Cognitive impairment develops when their weight exceeds the resilience of the brain, which is in turn determined by protective factors of genetic and environmental origin ”.
In the case of patients with cardiovascular disease, risk prevention (hypertension, obesity, etc.) in people who have never had a heart attack or stroke leads to a very significant reduction in the number of cases in subsequent years. On the contrary, such treatment after a stroke or heart attack brings only minimal benefits in terms of recovery: “In our opinion, the same reasoning should apply to Alzheimer’s disease: it is essential to treat people at risk before symptoms appear ”.
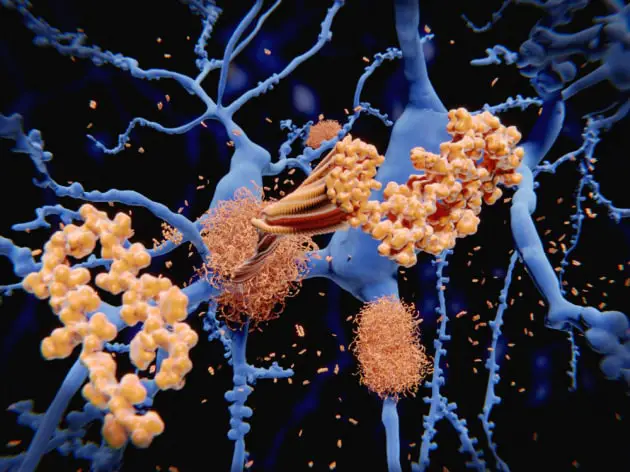
Identifying people at risk has so far required expensive and invasive procedures such as positron emission tomography (PET) and lumbar punctures. But the recent development of tools capable of detecting the presence of beta-amyloid and hyperphosphorylated tau in the blood is about to change this situation and could allow the inclusion of such screening in routine checks.
“Although patient management will not change overnight, a more detailed understanding of biological mechanisms at work will make it possible to develop more precise research protocols that take into account the different forms of Alzheimer’s disease “, say the authors.
This analysis is in line with the work done by the professor Bruno Dubois at the‘INSERM, co-author of this study, aimed at applying precise clinical diagnostic criteria. “In the years to come, we hope to adapt prevention and therapeutic strategies to each individual, rather than according to a standardized protocol that has already shown its limits “.
#Alzheimers #disease #identified #forms #disease






