There diabetic retinopathy, a progressive eye disease and unfortunately a major cause of blindness, it can be recognized thanks to the blue light that can be used to probe the depths of the eye and discover its areas: to declare it was a research team from Tokyo Medical and Dental University (TMDU) who has developed a comprehensive, non-invasive imaging technique. (1)
There Research was published in the scientific journal ‘Asia-Pacific Journal of Ophthalmology.
Blue light imaging technique to identify diabetic retinopathy: here’s how it works
Researchers from the Tokyo Medical and Dental University (TMDU) revealed that blue images obtained from multi-color widefield scanning laser ophthalmoscopy (SLO) can be used to identify areas of damage induced by diabetic retinopathy (DR) in a larger portion of the eye than with previous methods.
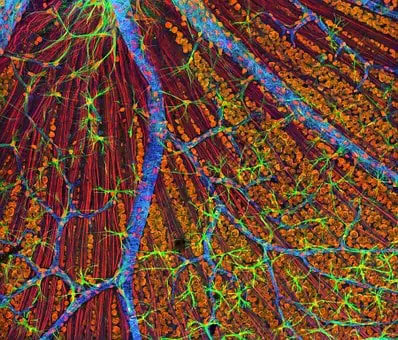
Current eye imaging methods include fluorescein angiography, which involves injecting dye into the eye. SLO is a non-invasive approach that does not require dye and Multi-color widefield SLO represents an advancement of this technique in which red, blue and green lasers are used to simultaneously capture images of a large portion of the eye.
Previous research has shown that blue images captured by conventional SLO can reveal low-reflective areas in the eye indicative of damage associated with DR. TMDU researchers sought to further evaluate this finding using the widefield SLO.
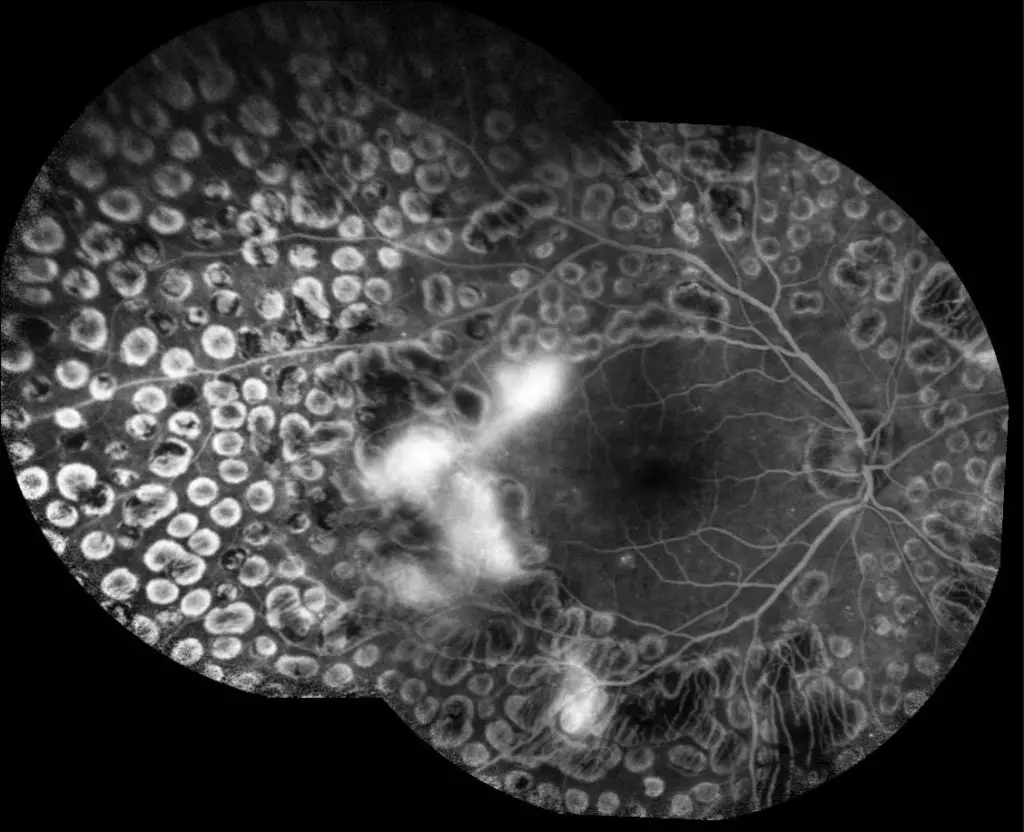
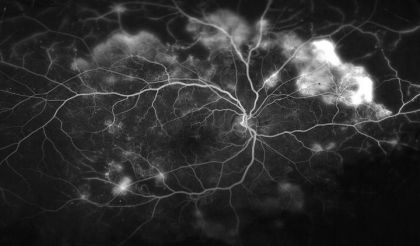
During this research, experts compared widefield blue SLO images and fluorescein angiography images taken in people with diabetes. The morphology of the retina was also evaluated in some subjects with DR.
“We found that the low-reflective areas in blue wide-field SLO images appeared to match the ischemic areas in the fluorescein angiogram images of DR patients “, explains Kyoko Ohno-Matsui, senior author. “We were delighted to find that the concordance rate was high ”.
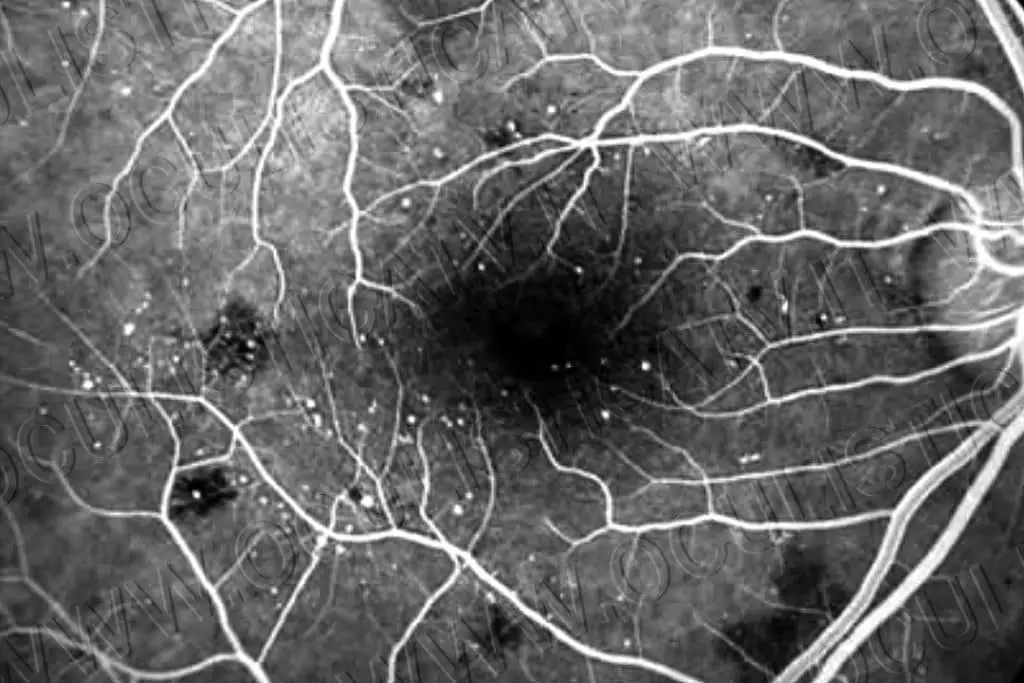
Further evaluation of the patient images showed that the ischemic areas, that is, areas of reduced blood flow, appeared to correspond to parts of the retina that were thin and partially disorganized.
“It is possible that the blue wavelength of light can pass more easily through these thinned areas of the retina, which appear as hypo-reflective areas in SLO images “, says Horie.
This study confirms the usefulness of blue widefield SLO as a simple and non-invasive tool for detecting eye damage associated with DR. This technique can serve as an important means of screening and monitoring disease progression in individuals with DR.
What is diabetic retinopathy?
Diabetic retinopathy is a complication of diabetes caused by high blood sugar levels that damage the back of the eye (retina). It can cause blindness if undiagnosed and untreated. However, it usually takes several years for diabetic retinopathy to reach a stage where it could threaten vision.
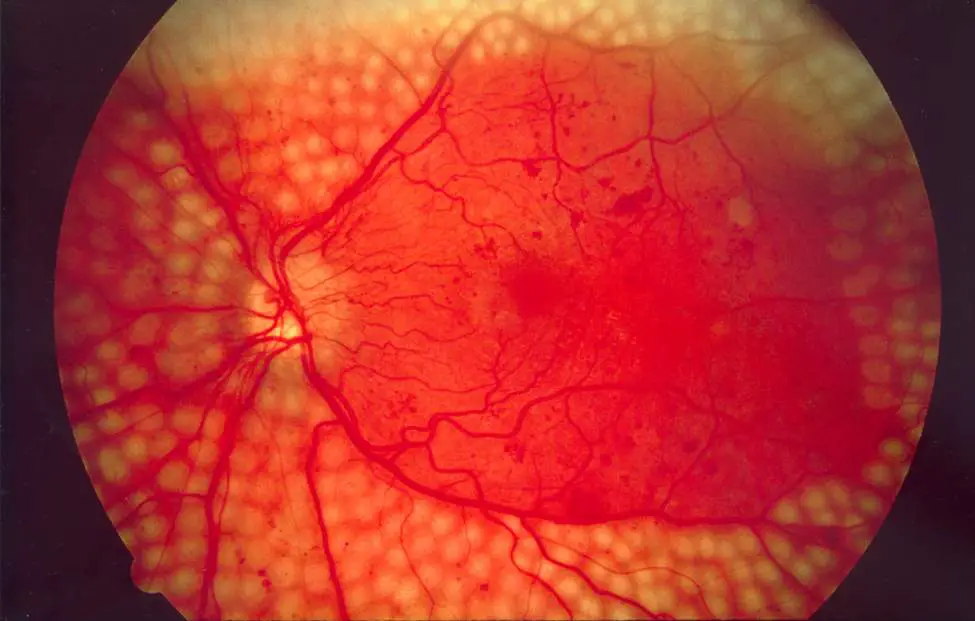
To minimize the risk of this happening, people with diabetes should:
- make sure they check blood sugar levels, blood pressure and cholesterol;
- Attend Diabetic Eye Screening Appointments: Annual screening is offered to all people with diabetes aged 12 years or older to promptly detect and treat any problems.
The retina is the layer of photosensitive cells in the back of the eye that converts light into electrical signals that are sent to the brain which transforms them into the images we see. It needs a constant supply of blood, which it receives through a network of tiny blood vessels. Over time, a consistently high blood sugar level can damage these blood vessels in 3 main stages:
- R.etinopathy basically: small swellings develop in the blood vessels, which may bleed slightly but do not usually affect vision.
- R.etinopathy pre-proliferative: more severe and widespread changes affect blood vessels, including more significant bleeding in the eye;
- R.proliferative ethinopathy: scar tissue and new vessels blood vessels, which are weak and bleed easily, develop on the retina, which can cause some loss of vision.
It is important to point out that if an eye problem is detected early, lifestyle changes and / or treatment can prevent it from getting worse.
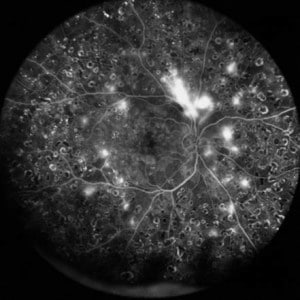
Anyone who has the type 1 diabetes or the type 2 diabetes is potentially at risk of developing diabetic retinopathy. The risk is greater if:
The affected person has had diabetes for a long time;
- The affected person has a persistently high blood sugar (glycemic) level;
- The affected person suffers from high blood pressure;
- The affected person has high cholesterol;
- It is a potentially pregnant woman;
- These are individuals of Asian or Afro-Caribbean origin;
As for the symptoms, early stage diabetic retinopathy does not tend to have noticeable symptoms until it is at a more advanced stage. However, the first signs of the condition can be detected by taking photographs of the eyes during diabetic eye screening. In principle, care should be taken if:
- Gradually deteriorating vision;
- Sudden loss of vision
- Floating shapes in your field of vision;
- Blurred or irregular vision
- Eye pain or redness.
These symptoms don’t mean it’s necessarily diabetic retinopathy, but it’s important to get them checked. Do not wait until a possible next screening appointment. All diabetics 12 years of age and older are advised to undergo eye screening once a year.
Screening is offered because:
Diabetic retinopathy does not tend to cause any symptoms in the early stages;
The condition can cause permanent blindness if not diagnosed and treated promptly;
Screening can detect eye problems before they begin to affect vision;
If problems are identified early, treatment can help prevent or reduce vision loss.
The screening test involves examining the back of the eyes and taking photographs. Depending on the outcome, you may be advised to return for another appointment a year later, attend more regular appointments, or discuss treatment options with a specialist. In fact, treatment for diabetic retinopathy is only necessary if screening detects significant problems that indicate your vision is at risk.
The main treatments for more advanced diabetic retinopathy are: laser treatment; injections of drugs into the eye; an operation to remove blood or scar tissue from the eyes.
Being a disease linked to diabetes, It is estimated that around 72 million of the world’s adult population (around 8.2%) have diabetes and that around one fifth of all adults with diabetes live in Southeast Asia.. In India, approximately 65 million people have diabetes. As the global prevalence of diabetes increases, the number of people with diabetes-related complications, such as DR, will also increase; it is likely that nearly a third of them will develop this complication.
The International Diabetes Federation (IDF) estimated that the world population with diabetes mellitus (DM) is 463 million in 2019 and will rise to 700 million in 2045. Diabetic retinopathy remains a common complication of DM and a leading cause of preventable blindness in the active adult population.
Globally, the number of people with DR has increased from 126.6 million in 2010 to 191.0 million by 2030 and it is estimated that the number with vision-threatening diabetic retinopathy (VTDR) will increase from 37.3 million to 56.3 million, if action is not taken promptly. Despite growing evidence documenting the efficacy of routine DR screening and early treatment, DR often leads to poor vision and is the leading cause of blindness in working-age populations.
DR has been neglected in health research and planning in many low-income countries, where access to qualified eye care professionals and tertiary eye care services may be inadequate.
#Diabetic #retinopathy #blue #light #intercepts #affected #areas







