The doctor Sarah Headlandtogether with colleagues of the Genentech Immunology Division in Southern San Franciscohe found, in a recent Researcha molecule that can trigger a form of severe asthma and that could be the piece of a puzzle useful for developing a new therapy that is more effective than the existing ones.
The results of the study have been published in the scientific journal Science Translational Medicine.
Severe asthma: a hope for therapy
The new study not only sheds light on the causes that cause severe asthma in certain individuals, but further highlights how the bacterial dysbiosisthe disruption of beneficial bacteria during exposure to pathogens affects vulnerable lungs.
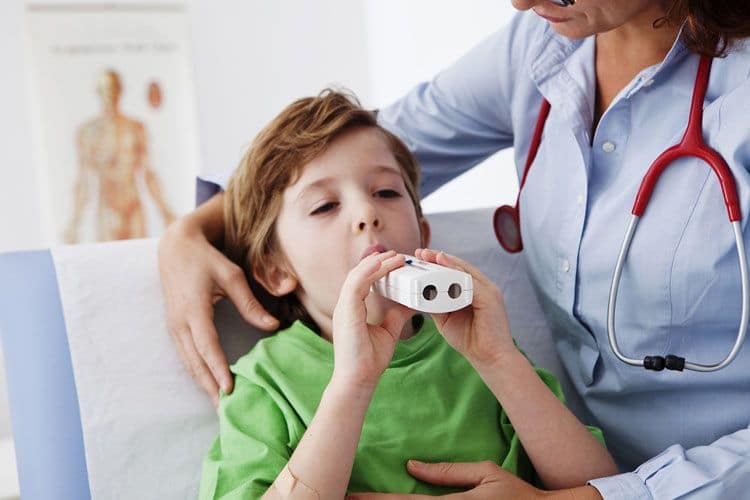
As the study progressed, the researchers were already aware that bacterial molecules could trigger inflammatory activity in the airways of the lungs because people with severe asthma undergo frequent changes in their bacterial populations. However, the exact mechanisms by which bacteria exacerbate asthma have remained unclear.
In search of answers, Dr Sarah Headland and her team focused on one form of asthma known as non-type 2 to find out why it is one of the most serious forms of inflammatory respiratory disease. She and her team have also begun the complex project of developing personalized therapy.
The study team explained that conducting a thorough study allowed a better understanding of this form of severe asthma and made it possible to create a draft of a targeted therapy specifically for patients with non-type 2 asthma.. The experts began by analyzing the cells and tissues of patients burdened with severe bacterial-associated asthma and comparing these results to the cells and tissues of people with mild to moderate forms of asthma and those who do not have asthma at all.
Headland and colleagues studied airway biopsies of 57 patients with severe asthma, 28 patients with mild or moderate asthma, and 16 healthy individuals. The key finding was the abnormally high activity of oncostatin M, a protein associated with inflammation and an aggressive immune response, unique among patients with severe asthma. Furthermore, exposure to lipopolysaccharide (LPS, a component of bacterial cell walls) triggered the activity of oncostatin M.
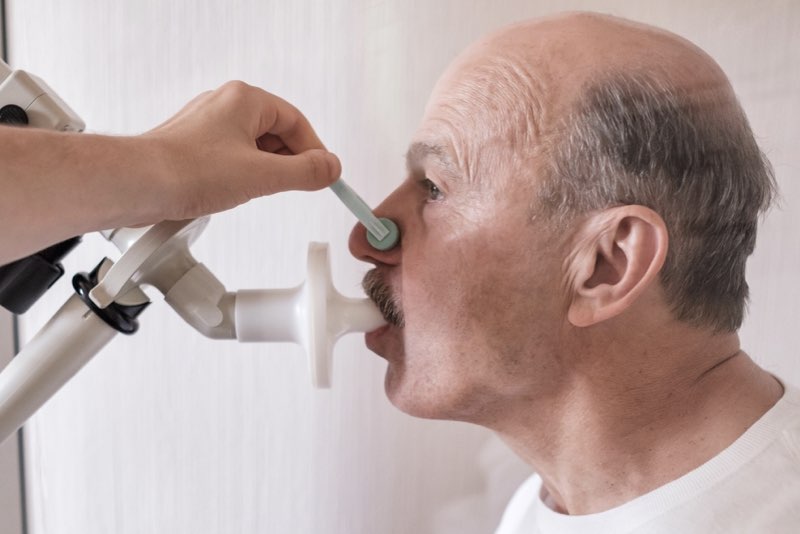
“Bacterial dysbiosis and opportunistic bacterial infections have been observed and may contribute to more severe asthma “Headland wrote in his study: “However, the molecular mechanisms driving these exacerbations remain unclear. We show here that bacterial lipopolysaccharide induces oncostatin M and that airway biopsies from patients with severe asthma show an OSM-driven transcription profile “
“This profile is related to the activation of inflammatory and mucus-producing pathways, “added Headland, noting that by using” primary human lung tissue or human epithelial and mesenchymal cells, we demonstrate that oncostatin M is necessary and sufficient to drive characteristics pathophysiological conditions observed in severe asthma after exposure to LPS “explained the scientist.
While the new analysis helped scientists better understand the factors behind severe bacterial-associated asthma, their research also suggested that a monoclonal antibody may one day block oncostatin M. Both lines of research, discovering the missing link in severe cases bacterial-associated asthma and identifying a potential form of treatment provide a ray of hope for patients with the form of the disease widely known as non-type 2.
It was once thought that asthma was a single disorder, but now experts have understood that it is several complex but correlated conditions with varying underlying triggers. There are two key categories of severe asthma: type 2 inflammation and non-type 2 inflammation. Each of the two categories is based on the biological mechanisms that drive the disease. Type 2 inflammation, for example, includes allergic asthma and eosinophilic asthma.
The Asthma and Allergy Foundation of America defines allergic asthma as an inflammatory disease caused by an allergen, such as exposure to cockroaches, pollen, dust mites, mold, or pet dander, just to name a few triggers. The immune system responds by producing an overabundance of immunoglobulins (antibodies) known as immunoglobulin E or IgE. Extremely high levels of IgE can cause inflammation of the airways of the lungs.
Another type 2 form is eosinophilic asthma, characterized by high levels of white blood cells known as eosinophils. A hallmark of this type of asthma is generalized swelling throughout the respiratory tract, from the nasal region to the smallest airways in the lungs. People with this form of asthma experience wheezing, shortness of breath, chest tightness, and abnormal lung function, among other symptoms.
Non-type 2 inflammation in severe asthma was defined as the absence of eosinophils. However, doctors say there is much more to this form of asthma, which is characterized by a constellation of problems, ranging from an extreme inflammatory condition in the lung airways to shortness of breath and difficulty in controlling the condition.
In terms of treatment, medical experts have also long known that non-type 2 inflammation does not respond to inhaled corticosteroids, a standard of care that works well in other forms of asthma. Thus, the discovery of oncostatin M-associated bacterial dysbiosis opens a new window of understanding on a debilitating form of the disease, Headland and colleagues reported.

Indeed, there is an obvious unmet need for patients with this form of asthma because there is no specific therapy, something targeted, to address the unique manifestations of this form.
Headland and his collaborators found that oncostatin M drives key features of asthma, such as inflammatory signaling and excessive mucus production, when exposed to LPS or a common bacterial pathogen, Klebsiella pneumoniae.. And because of the unique role played by oncostatin M, Genentech scientists are developing a potent monoclonal antibody that can block the protein, staving off inflammation in the airways.
So far, the tests, which look promising, have been conducted on a mouse model. The hope is to develop a treatment that can be tested in a human clinical trial. “Together, these findings provide scientific rationale to support the clinical development of therapies aimed at[oncostatina M] to prevent the progression of asthma“, Concluded the authors.
#Severe #nont2 #asthma #missing #link #therapy










