Almost every type of liver cancer develops after decades of chronic liver disease, but a new discovery by Columbia researchers could lead to treatments that could disrupt the chronic course of liver disease.
The new research has shown that during chronic liver disease a shift in the balance of quiescent and activated stellate liver cells not only promotes fibrosis, but also sets the stage for the most common type of primary liver cancer, called hepatocellular carcinoma.
The results of the study have been published in the scientific journal Nature.
Here’s how to prevent liver cancer from developing
According to the new research, it may be possible to prevent the development of liver cancer, the fourth leading cause of cancer death in the world, by interfering with the activation of stellate cells. Hepatocellular carcinoma develops almost exclusively in patients with chronic liver disease, including cirrhosis, hepatitis, or non-alcoholic fatty liver disease. These diseases often cause extensive and progressive scar tissue (also known as fibrosis) in the liver.

“Although fibrosis almost always precedes cancer, little is known about the causal relationships between the two and how we might be able to stop this process.Said Robert F. Schwabe, MD, Professor of Medicine and Director of the Digestive and Liver Disease Research Center at Columbia University’s Vagelos College of Physicians and Surgeons, who led the study.
Schwabe and his team focused on the stellate cells of the liver, so named for the multiple protrusions that give them a star-like shape, because they are heavily involved in liver fibrosis. After developing new genetic tools that allow researchers to manipulate and analyze star cells in mice, Schwabe found that the population of these cells changes as cancer develops.
“In a healthy liver, stellate cells are quiescent and express factors, especially hepatocyte growth factor, which protect the organ“, Explained the scientist:”In the presence of chronic liver disease, however, the number of protective quiescent stellate cells decreases as more stellate cells become activated.“.
Activated cells express factors that promote tumors, particularly collagen, the building block of scar tissue. This dynamic shift from protective to tumor-promoting cells sets the stage for liver cancer. The same imbalance in stellate cells and its association with an increased risk of cancer development has been observed in patients with liver cancer, suggesting that the same process occurs in people.
Hepatocellular carcinomas are typically detected too late to be cured, and most patients die within two years of diagnosis despite new, more effective medical therapies such as the combination of atezolizumab and bevacizumab. The incidence of hepatocellular carcinoma has tripled over the past 30 years and is projected to increase further due to the increase in rates of nonalcoholic fatty liver disease caused by increased obesity.
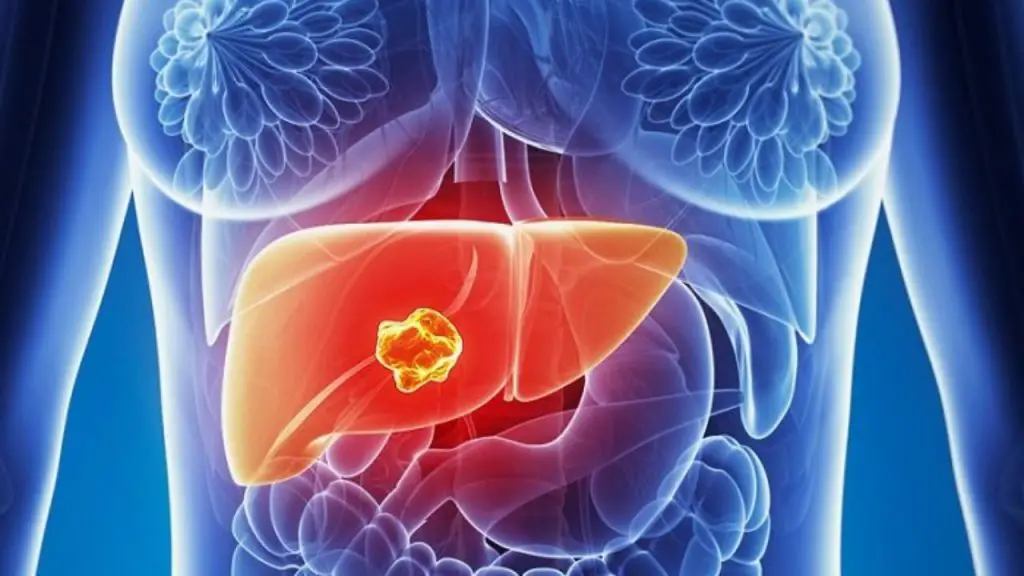
The discovery raises the prospect of preventing liver cancer by restoring the normal balance of stellate cells: “I don’t think we will be able to cure cancer by restoring the balance of the stellate cells“Says Schwabe. “Activated stellate cells create an environment conducive to cancer development, but do not appear to play a role in cancer progression once the tumor has developed“.
“But restoring cell balance or associated mediators in people with chronic liver disease can reduce the risk of developing cancers in the first place. This would be a huge benefit for the many millions of people with chronic liver disease, who have a high chance of developing liver cancer.“.
Professor Luigi BolondiProfessor of Internal Medicine at the University of Bologna, Director of the Complex Unit of Internal Medicine at the Policlinico S. Orsola Malpighi of Bologna, internist who mainly deals with liver diseases, in particular the diagnosis and treatment of primary liver tumors, has declared: “A tumor is any formation with abnormal anatomical features within an organ“.
“In the liver, as in any other organ, benign and malignant tumors can develop. Malignant tumors have the characteristic of growing abnormally, invading and subverting the surrounding tissue, also causing lesions in other organs that are called metastases. Among the malignant tumors of the liver, the most frequent is Hepatocarcinoma, which occurs almost exclusively in patients with chronic liver diseases, of viral and non-viral origin.“.
“By “nodule” we mean a formation of an indeterminate nature found, generally with an imaging technique (ultrasound, CT scan or MRI), in the context of the liver. In patients with chronic liver disease, when a “nodule” is found, it is necessary to carry out other tests to arrive at a definitive characterization, since, until proven otherwise, each nodule is suspected for malignancy. However, it should be remembered that the distinction is not always easy as the malignant transformation process is complex and there may be intermediate forms (dysplastic nodules) which are not yet malignant tumors but can become malignant.“.
“Malignant tumors generally arise in the cirrhotic liver. However, it is possible, in a limited number of cases, that they can also arise on chronic hepatitis. This is more common in patients with hepatitis B. Ultrasonography, performed at regular intervals (every 6 months) in patients with liver cirrhosis, in patients with advanced and severe fibrosis and in patients with hepatitis B, is the most common technique. frequently leads to the discovery of the suspicious lump. When the lump has been discovered, it is necessary to investigate further with further investigations“.
“To understand if a nodule is malignant it is necessary to evaluate its appearance after administration of contrast medium to study its vascularization. The first technique that is usually used in Italy is ultrasound with contrast medium (CEUS). If this does not clarify it is necessary to perform a CT scan or an MRI with contrast medium“.
“These tests are also necessary for “staging”, that is to understand if there are other nodules in the liver (possibly not visible on ultrasound) and if there has also been involvement of the intrahepatic vascular structures. It should be remembered that MRI is the technique with the greatest diagnostic accuracy. It can also make use of hepatospecific contrast media that can provide additional information in poorly vascularized nodules.“.
“However, despite all the investigations, it is not always possible to clarify the nature of the nodule (whether benign, dysplastic or malignant), especially in small nodules (<1cm or <2cm). In these cases, an ultrasound-guided liver biopsy is required. It is advisable to perform an ultrasound every 6 months. A longer interval exposes the patient to the risk of finding larger nodules and therefore more difficult to treat with radical interventions“.
“Patients who have cleared the C virus should also continue the ultrasound surveillance program, as the risk of developing nodules is decreased but not completely eliminated. The risks are believed to be greater for patients with a longer history of the disease or with advanced fibrosis or cirrhosis. In any case, the recommended interval is always 6 months“.
According to the AIRC: “The incidence of liver cancer varies greatly depending on the geographical area: it is more common in Asia than in the United States and Europe. It is the sixth most common cancer worldwide and the second leading cause of cancer death: in 2012 over 700,000 people died of liver cancer worldwide“.
“In Italy it is rarer: it is estimated that approximately 8,900 primary liver tumors are diagnosed each year in men and 4,000 in women (Italian Cancer Registry 2017), with a ratio of about 2 to 1 between men and women. In men, the incidence increases rapidly with age: it goes from 3 per 100,000 cases under the age of 45, to 32 per 100,000 in people aged between 60 and 64, up to 62 per 100,000 over 75 years.“.
“On the other hand, secondary tumors are more frequent, i.e. metastases that colonize the liver from other organs. The liver, in fact, due to its function as a filter of the organism, receives blood from almost all body parts and therefore is easily the site of metastases of other tumors that find in the liver a favorable site for their development.“.
“The exact mechanism by which liver cancer develops is not yet known and many points remain to be clarified. Some elements, however, are sure risk factors: liver viruses type B and C, which are transmitted through blood or sexual intercourse or from mother to child during pregnancy. Viral hepatitis often does not cause any symptoms, although their presence is easily detected by a blood test“.

“Infection with virus B, however, can be prevented with a vaccine that is now administered to all newborns and is still useful at any age. If hepatitis becomes chronic it can cause tumor degeneration of hepatocytes even after many years. Very effective drugs are available against hepatitis C that should over time reduce the number of cases of this disease and consequently the number of tumors.“.
#Liver #cancer #prevention #strategies #arrive












