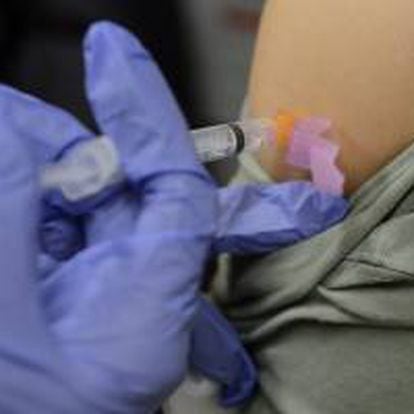
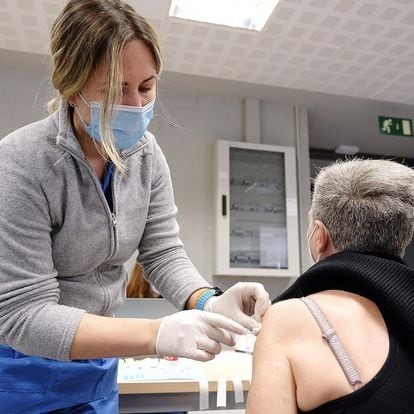
The Ministry of Universities estimates that 53.5% of permanent teaching staff will be able to retire in the next 10 years. In many branches of knowledge it is not a big problem – there are some 15,000 researchers with accredited merits to take over – but in the field of Medicine a real drain is taking place. Among doctors, retirement goes twice as fast: in the next five years 43% of teachers will leave their post, a percentage that rises to 55% in the case of those who also work in hospitals or outpatient clinics. The situation is further aggravated if one takes into account that very few of the practicing doctors are accredited to join the civil service as full professors. For this reason, the Ministry of Universities and the National Agency for Quality Assessment and Accreditation (Aneca) are preparing shock measures.
In the Department of Surgery of the University of Cádiz there are no professors left – not even in Maternal-infantile and Radiology -, there are four holders and a score of associate professors who give practical and theoretical classes. “The associates are under the umbrella of the incumbents, if they retire, they cannot be”, explains Luis Miguel Torres, one of the incumbents. Like him, the other three full professors of the faculty are over 60 years old and none of the young people has yet to be credited. “The first thing Aneca looks at is the number of publications in high-profile magazines. What does it matter to the student if what he wants is a good class? They had to look at the opinions of the students, the classification in the MIR … ”, considers Torres.
The doctors who teach at the University – there is a minority who only work in the faculty – do not have time for teaching, for research and, in addition, to operate or visit a health center. José Luis Aguayo is 66 years old and until three years ago he was not accredited as Professor of Surgery at the University of Murcia, despite his almost 400 publications (half in high-impact journals) and his special interest in teaching. “It is nonsense, [obtener la cátedra] when I am about to leave, I would have to be a professor at 40 ”, he reflects.
At the University of the Balearic Islands, for example, there are only two professors and one tenured. Its dean, the psychiatrist Miquel Roca, explains that the first class has not yet graduated and that there are doctors with publications behind them and a great practical experience who lack hours of teaching to be able to obtain accreditation. “In two years we will have four or five, but they are few,” he laments.
In Medicine there is no training itinerary to be a teacher, as in other fields – there is no assistant figure – so you have to finish the MIR and accumulate class hours before you can get accredited. “An associate doctor can be 20 or 30 years charging 300 euros to teach a few hours of class a week and after that time, if he has been able to investigate and sign articles in his hospital, he is credited as the holder”, explains Aguayo, chief from the Surgery Service of the Morales Meseguer University Hospital in Murcia. 30 years ago, when in Spain there were not so many medical schools and health and educational competences had not been transferred, in hospitals in Madrid, Santiago, Barcelona or Granada there were itineraries to be a teacher from the base designed by the State. Therefore, there is a lack of incentives for the training of new teachers. Whoever takes the step is by pure vocation.
“The situation is unsustainable”
Data from the ministry show the dramatic situation: there are 18 professors of Pediatrics for 43 faculties, in five years 29% of surgeons who are full professors (from 117 to 83) have been lost and more than half (52%) of gynecologists from the same body, who have gone from 45 to 22. The conference of deans presents a worrying panorama in its latest report: “In 2019 there has been an average of only one accreditation to a full professor per faculty (there are 43 centers ) to be distributed among 25 areas of knowledge with teaching in the degree of Medicine. Very few apply for accreditation, but fewer still obtain it. The situation is unsustainable ”. If we go into detail, in 2019 only 14 doctors from preclinical (0.33 per center), 26 from clinic (0.61 per center) and 86 from health specialties (two per center) were accredited, but in the latter This section includes veterinarians, pharmacists, physiotherapists and nurses.
The mathematician Mercedes Siles, director of Aneca, has been involved in the matter: “We are concerned that they are running out of teachers. So we have created a commission with the deans and deans of Medicine. More must be counted on the merits [para la acreditación] what you are doing in the hospital part. The healthcare component has to be valued more ”. The Aneca and the conference of deans have until December to agree on the criteria for accreditation, because in January they have to be published.
Pablo Lara, dean of Medicine at the University of Malaga and president of the deans, believes that the distribution of hours should be maintained – a third of the day is dedicated to the university – because it is vital that doctors continue to have contact with patients and get to know the latest clinical news to pass on to students. But he also argues that formulas should be sought so that not only scientific but professional merits are valued in the accreditation, such as the practice of a new technique when operating.
Javier Arias, dean of Medicine at the Complutense de Madrid (UCM), sees the solution difficult because he considers that subjectivity prevails in the granting of accreditation. “What for one is new, for another, no. It’s like when a new operative technique appears in a newspaper that has actually been used for a long time, but someone has thought of it being known ”, he argues. The Complutense is a very old university, but Arias assures that they have a waiting list of accredited doctors to teach. Large hospitals with powerful research ―Clínico, Gregorio Marañón and 12 de Octubre― are associated for training at the UCM and this is a pole of attraction for teachers.
Carmen Gallardo, dean of the Rey Juan Carlos University of Madrid and who also participates in the negotiations with Aneca, believes that it would give them “a break” that all the autonomous governments ―Andalucía or Galicia already have it― establish the figure of the contracted doctor (with the doctorate degree), as exists in other branches of knowledge, as it requires less merit to be accredited. But in that case, the doctor may lose salary compared to what he has paid entirely for the hospital. That is the brake for many doctors in Cádiz. “It doesn’t compensate them, it discourages them,” Torres explains. In Madrid, it is being negotiated.
Gallardo emphasizes that there is interest: “It is in the DNA of a doctor to teach as he was taught and in the faculties and hospitals there has been a lot of promotion for doctors to get doctorates.” The surgeon Torres, from Cádiz, disagrees: “In a scale of OPE [oferta de empleo público], right now it counts the same to do the thesis as to go to four congresses. It has been greatly devalued ”. Siles has pending to speak with the Ministry of Health about this depreciation of the academic task.
The cap also affects six-year terms, the salary supplements that reward the work of all teachers with a permanent position. Siles explains: “In the six-year period of transfer, the assistance part will also be taken into account when the Aneca call comes out.”
Next year the degree in Medicine will be inaugurated at the University of Almería and, from its faculty, they assure that the first courses are “covered” with teaching staff. They will soon have their first Ph.D. professor, a woman who has already been accredited. The problems will come in a couple of years. Now it is the University of Jaén that is queuing to implement the degree in Medicine. It already has the endorsement of the Junta de Andalucía and predictably the opposition of the deans, who believe that there are excess training centers.