A team of scientists of the Cedars-Sinai Board of Governors Regenerative Medicine Institute, observing some stamina cells, revealed the origins of a municipality ovarian cancer developing fallopian tube tissues in the laboratory, allowing them to characterize how a genetic mutation exposes high-risk women to this cancer.
The fabrics created, known as organoids, have the potential to predict which individuals will develop ovarian cancer years or even decades earlier, enabling early diagnosis and prevention strategies.
The results of the Research have been published in the scientific journal Cell Reports.
Ovarian Cancer Prevention: Here’s What Research Says
Ovarian cancer is the leading cause of gynecological cancer deaths in the United States, partly because symptoms are often unnoticeable and most cancers evade detection until they are in advanced stages and have spread beyond the ovaries.
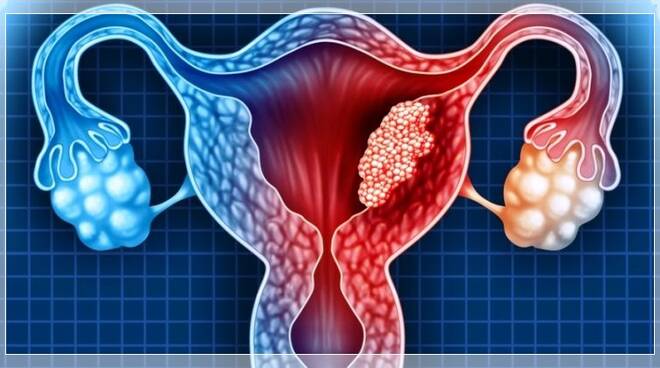
The lifetime risk of developing ovarian cancer is less than 2% for the general female population, the estimated risk for women carrying a mutation in the so-called BRCA-1 gene is between 35% and 70%, according to the ‘American Cancer Society.
Faced with such high odds, some women with BRCA-1 mutations choose to have their breasts or ovaries and fallopian tubes surgically removed even though they may never develop tumors in these tissues.
The new study results could help doctors identify which of these women are more likely to develop ovarian cancer in the future, and which are not, and pursue new ways to block the process or treat the cancer.
“We created these fallopian organoids using cells from women with BRCA-1 mutations who had ovarian cancer“, has explained Clive Svendsen, Ph.D., executive director of the Cedars-Sinai Board of Governors Regenerative Medicine Institute. “Our data supports recent research indicating that ovarian cancer in these patients actually begins with cancerous lesions in the linings of the fallopian tubes. If we can detect these anomalies early on, we may be able to short-circuit ovarian cancer. “
Svendsen, professor of biomedical sciences and medicine, is the corresponding author of the new study, conducted at Cedars-Sinai. The other corresponding author is Beth Karlan, MD, professor of obstetrics and gynecology at the David Geffen School of Medicine at UCLA and director of cancer population genetics at UCLA Jonsson Comprehensive Cancer Center.
To make their discoveries, the research team generated induced pluripotent stem cells (IPSCs), which can produce any type of cell. They started with blood samples taken from two groups of women: young ovarian cancer patients who had the BRCA-1 mutation and a control group of healthy women. The researchers then used iPSCs to produce organoids that mimic the lining of the fallopian tubes and compared the organoids in the two groups.
“We were surprised to find more cellular pathologies consistent with cancer development only in the organoids of BRCA-1 patients “, he has declared Nur Yucer, Ph.D., project scientist in the Svendsen laboratory and first author of the study: “Organoids derived from women with the most aggressive ovarian cancer showed the most severe organoid pathology ”.
In addition to showing how ovarian cancer is “sown“In the fallopian tubes of women with mutated BRCA-1, organoid technology can potentially be used to determine whether a drug could work against the disease in an individual, Svendsen said.
Each organoid carries the genes of the person who provided the blood sample, making it a “twin”Of that person’s fallopian tube linings. It is possible to test multiple drugs on organoids without exposing the patient to them.
“This study represents an exciting use of IPSCs, bringing us closer than ever to significantly improving outcomes for women with this common type of ovarian cancer,” he has declared Jeffrey Golden, MD, deputy dean of university research and education and director of the Burns and Allen Research Institute in Cedars-Sinai.
“Building on these findings could one day allow us to provide an early and lifesaving diagnosis of ovarian cancer in women carrying the BRCA-1 mutation and create effective and individualized prevention and treatment strategies as needed.“, Concluded the scientist.
According to a recent study that collects data from 1,000 women in 39 countries, The number of women diagnosed with ovarian cancer is likely to rise to 371,000 new cases per year by 2035.
There is currently no easy way to perform an accurate ovarian cancer screening. The most common symptoms – including discomfort in the abdomen or pelvic area, persistent bloating, loss of appetite, needing to urinate more often or more urgently – are sometimes misdiagnosed as gastrointestinal upset. For this reason, most patients are identified only in the advanced stages, when the disease becomes more difficult to treat.
Raising awareness of ovarian cancer symptoms and risks among the general public could help reduce delays in diagnosis. Two-thirds of the women surveyed in the study Every Woman they had never heard of ovarian cancer or knew anything about it. A quarter waited three months or more before seeing a doctor with their symptoms and one in 10 waited more than six months. Those who contributed directly to their healthcare costs were less likely to seek medical help.
Consulted as part of the study, gynecologist oncologist Dr Manas Chakrabarti described the devastating impact of late diagnosis: “In most cases (presenting as an emergency) the patients are not fit enough to receive any part of the management path – to see the good effect of the treatment we must be able to make the patient endure the two treatment modalities , but in many cases general health does not allow it, so we are defeated in the first place, a shocking fact for both patients and us ”.
By combining data from two Education, it is estimated that one in six women will lose their life within three months of being diagnosed with ovarian cancer. Ovarian cancer unfortunately has the lowest survival prospects of all cancers that affect women, with five-year survival rates of between 30% and 50%. By comparison, more than 80% of women with breast cancer will survive for five years or more in many countries.
The prognosis for long-term survival can be poor using traditional treatments such as surgery and chemotherapy. However, the ongoing development and identification of targeted therapies for gynecological cancers could revolutionize treatment and significantly increase survival rates for women with ovarian cancer.
New advances in microbiology have led to the development of targeted agents capable of identifying the signaling pathways of tumor cells, stroma and vascular system in tumor tissues.
Targeted therapies have opened up the possibility that someday there will be a cure for gynecological cancers. However, urgent action is now needed to reduce delays in diagnosis and offer women around the world the best chance of beating ovarian cancer.
#Ovarian #cancer #onset #discovered #highrisk #women







