A team of experts from the Georgia Institute of Technology, has designed, in a recent research, a new chip that will facilitate the treatment of metastatic tumors easier and faster. The detection method developed by scientists could revolutionize cancer treatment by showing how tumors metastasize and at what stage they are.
The results of the study have been published in the scientific journal Nature Communications.
New chip for the treatment of metastatic tumors: this is how it works
Neoplasms spread through the circulating cancer cells (CTCs) that travel through the blood to other organs and are nearly impossible to trace. The Georgia Institute of Technology research team has developed a detection method that could revolutionize cancer treatment by showing how tumors metastasize and at what stage they are. This important discovery could lead to earlier and more targeted treatment, starting with a simple blood test.
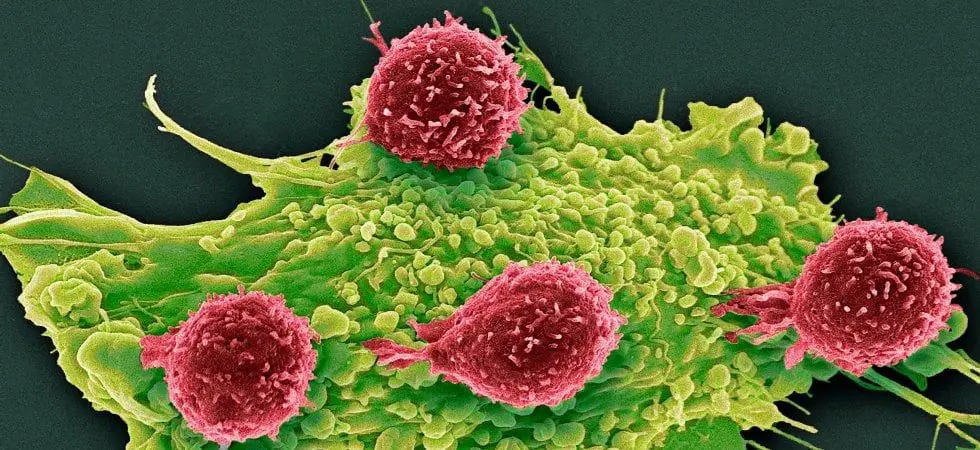
When a tumor begins to metastasize, it sheds its cells in the blood. A single cell often does not survive the bloodstream on its own, but the clusters of cells are much more armored and can travel to other organs, effectively bringing the cancer to a metastatic state.
CTCs have proved difficult to study, let alone the treatment. Blood contains billions of cells per milliliter and only a handful of those cells would be CTC in a patient with metastatic cancer. Such intense filtration was inaccessible using conventional laboratory methods. More traditional filtration is too aggressive and would break the cluster into single cells and ruin the ability to study the effect of a cluster.
“This is what interested engineers like me because we are really good at creating sensors or small devices that actually perform sensitive analysis,” he said. Fatih SariogluAssociate Professor of the School of Electrical and Computer Engineering: “We have started developing technologies to capture these precious cells to help better manage cancer.”
Sarioglu’s lab has created a new chip called Cluster-Well, which combines the precision of microfluidic chips with the efficiency of membrane filtration to find CTC clusters. Using micron-sized features, the new microfluidic chip can precisely intercept each cell in a blood sample and determine if it is a cancer cell.
“The new microfluidic chip gives you more control as a designer to actually ask any questions you want to ask those cells,” explained Sarioglu: “It increases accuracy and sensitivity, which is what you need for an application like this. because you want to find that single cell from many blood cells ”.

To rapidly process a clinically relevant volume of blood, the researchers relied on membrane filtration to make the chip’s operation more scalable. Indeed, the new chip looks like a standard membrane filter, but under the electron microscope the new microfluidic chip reveals its delicate structure used to capture clusters by letting other blood cells pass.
Convenience was as important as functionality to the researchers. Although the new chip is initially manufactured with silicon just like a central processing unit in a computer, it is later transferred to polymers to make it accessible, convenient and single-use, while maintaining its delicacy and precision.
“We’ve really only created the traps we need to recognize clusters with the new microfluidic chip, and the rest is just a standard portafilter,” said Sarioglu. “Compared to a conventional microfluidic chip, you get a much more practical test with orders of magnitude improvement in throughput and greater sensitivity.”
The team of experts used the new chip to examine blood samples from ovarian or prostate cancer patients through a partnership with Emory and Northside Hospitals. Researchers isolated clusters of CTCs ranging from two to 100 or more cells from individuals with prostate and ovarian cancer and used sequencing of RNA to analyze a subset.
The unique design of the new chip means that the CTC clusters are filtered in microwells and can subsequently be consulted for further analysis. Even a single CTC can contain a significant amount of data about the patient and their specific tumor, which can be critical for disease management. For example, the researchers noticed hundreds of CTCs in clusters in the blood of ovarian cancer patients, some still alive, a finding that could be a consequence of the spread of the disease.
Not only that, by sequencing RNA in prostate CTC clusters isolated from the new chip, the researchers identified specific genes expressed by these metastasizing cells. It is important to specify that CTC clusters from different patients have been shown to express different genes, which can potentially be used to develop personalized and targeted therapies. Sarioglu envisions Cluster-Wells being a routine part of the treatment process for determining what stage the cancer is at from a simple blood draw.
“Finding these clusters was very elusive,” conct Sarioglu: “But this is a technology that allows you to access these precious clusters of cancer cells circulating in virtually any cancer with precision and convenience that was not possible before.”
#chip #metastatic #cancer #treatment #easier #faster








