There diastolic dysfunction associated with individuals affected by rheumatoid arthritis it can be treated with new therapeutic approaches. This was declared by a team of researchers from Queen Mary University of London.
The new study was published in the scientific journal PNAS.
Diastolic dysfunction and rheumatoid arthritis: here’s what the research says
To date, individuals with rheumatoid arthritis are particularly predisposed to a type of heart failure called diastolic dysfunction., which can lead to heart failure, resulting in an increased mortality rate in people with RA.
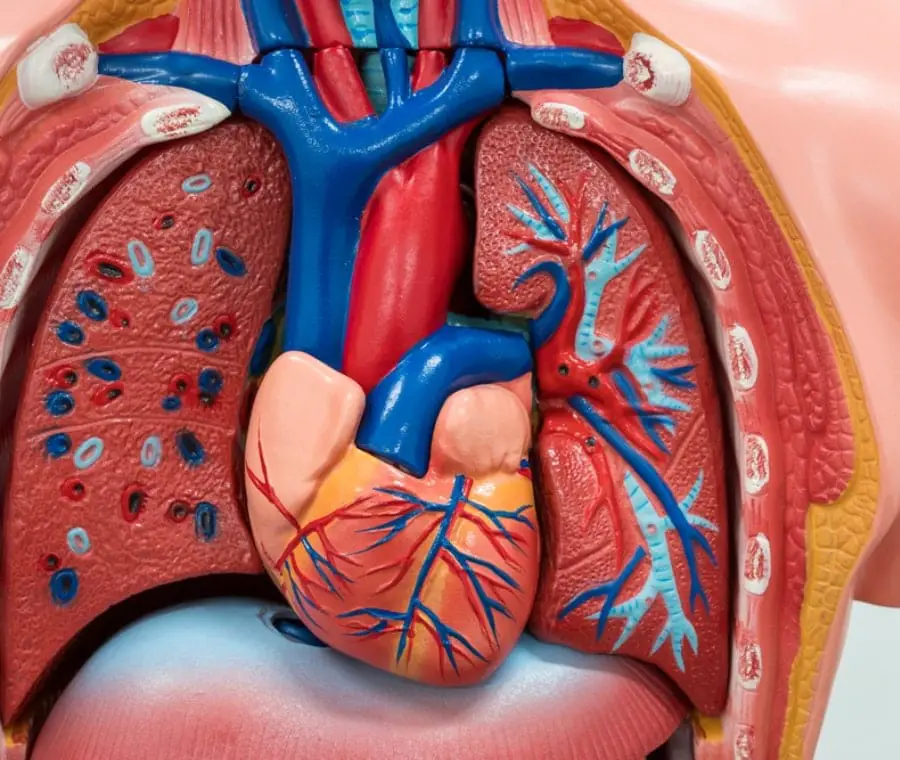
After several attempts, the Researchers at Queen Mary’s William Harvey Research Institute (WHRI) have successfully identified the right pattern by characterizing experimental animals with arthritis. The animals developed cardiac diastolic dysfunction, manifesting the symptoms presented by RA patients. Diastolic dysfunction means that the heart is able to contract normally but unable to dilate properly, leading to heart failure over time.
Professor Mauro Perretti, lead author of the study and professor of immunopharmacology at the Queen Mary University of London, he has declared: “As often happens, the description of a valid disease model can open new perspectives on pathogenetic mechanisms and on new therapeutic approaches. Currently, the cardiomyopathy of rheumatoid arthritis patients is not treated and, moreover, antirheumatic drugs do not cure the cardiomyopathy of rheumatoid arthritis patients ”.
“The large area of cardiac inflammation is largely unexplored. At WHRI we have several groups dealing with experimental and translational work on different cardiac syndromes. So, there is work on myocarditis, diabetes-induced cardiomyopathy and now with this study, diastolic dysfunction in inflammatory arthritis. The WHRI of Queen Mary University of London is a place of excellence to study cardiac inflammation in all its many faces, thanks also to our partnership with the Barts Heart Center at the Barts Health NHS Trust “, concluded the expert.
Diastolic dysfunction occurs when the diastolic part of the heart is abnormal. THE ventricles do not relax adequately and stiffen, which means they cannot fill adequately with blood. This causes blood to accumulate in other parts of the body.

The pressure in the ventricles then increases as blood from the next heartbeat tries to enter. This leads to extra pressure and fluid accumulation in the vessels of the lungs (called pulmonary congestion) or in the vessels leading back to the heart (called systemic congestion).
Pulmonary congestion causes fluid or transudate to leak from these vessels into the pulmonary alveoli, causing pulmonary edema. This condition hinders the oxygenation of blood in the lungs, causing shortness of breath and (in some cases) even death if the condition is not discovered and treated quickly.
Systemic congestion has detrimental effects on other organs in the body such as the kidney and liver, due to poor organ perfusion. Swelling and congestion can also occur in the legs and inside the abdomen.
Diastolic dysfunction is a common problem, with many people over the age of 70 having been affected by this morning. In most cases, the condition is not severe enough to lead to diastolic heart failure.Diastolic dysfunction itself often causes no symptomsHowever, if the problem progresses to the point that it begins to affect other organs and parts of the body, diastolic heart failure is diagnosed. In these situations, common symptoms include:
- Difficulty in breathing and shortness of breath. Initially, this may only occur during exercise, but as the disease progresses, breathing can become problematic during any activity, including resting or lying down;
- Unusual weight gain or swelling (edema) in the ankles, legs and abdomen;
- Irregular or rapid heartbeat.
Diastolic dysfunction is an early adverse prognostic factor in hypertension and is a reversible condition. Early diagnosis and treatment are needed to avoid heart complications. The objective of this study was to evaluate the onset of diastolic dysfunction in hypertensive patients referred for echocardiographic evaluation of left ventricular function in a secondary hospital.
Several factors were also evaluated such as age, sex, systolic and diastolic pressure, duration of hypertension, previous myocardial infarction or ischemic heart disease and finally a choice of antidepressant drugs that influence the development of diastolic dysfunction in hypertensive patients.







